 |
 |
- Search
| Chronobiol Med > Volume 4(4); 2022 > Article |
|
Abstract
Objective
Methods
Results
NOTES
Funding Statement
This research was supported by the Korea Medical Device Development Fund grant funded by the Korea government (the Ministry of Science and ICT, the Ministry of Trade, Industry and Energy, the Ministry of Health & Welfare, the Ministry of Food and Drug Safety) (RS-2020-KD000188) and a grant of the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), funded by the Ministry of Health & Welfare, Republic of Korea (No. HR21C0885).
Conflicts of Interest
Availability of Data and Material
The datasets generated or analyzed during the study are available from the corresponding author on reasonable request.
Author Contributions
Conceptualization: Jin Won Seo. Data curation: Minjeong Kim. Formal analysis: Jin Won Seo. Funding acquisition: Seog Ju Kim. Investigation: Minjeong Kim, Hyerin Gu, Hyeyeon Jang, Jin Won Seo. Methodology: Jin Won Seo. Project administration: Seog Ju Kim. Resources: Seog Ju Kim. Software: Minjeong Kim, Jin Won Seo. Supervision: Seog Ju Kim. Validation: Jin Won Seo, Seog Ju Kim. Visualization: Jin Won Seo. Writing—original draft: Jin Won Seo. Writing—review & editing: Seog Ju Kim.
Figure 1.
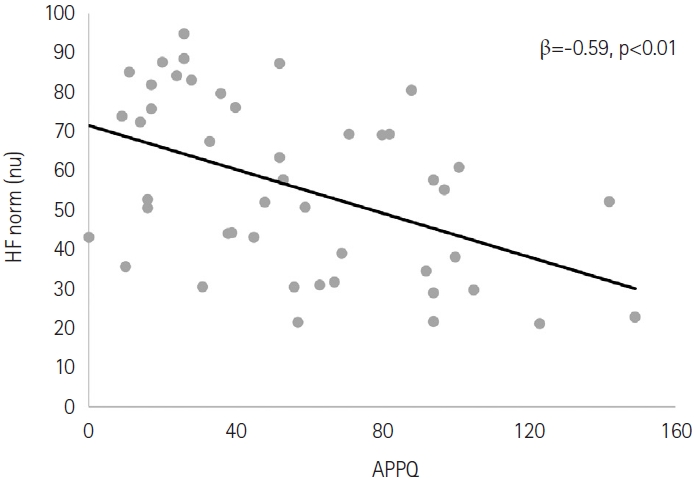
Table 1.
Table 2.
| Parameter | Value (n=46) |
|---|---|
| PSQI | 11.57±3.45 |
| BAI | 16.76±11.64 |
| APPQ | 56.17±37.15 |
| PSWQ | 44.74±11.77 |
| LSAS | 49.87±27.57 |
| TP | 5.44±1.12 |
| HF norm | 49.87±27.57 |
| LF/HF ratio | 1.12±1.03 |
Values are presented as mean±SD. PSQI, Pittsburgh Sleep Quality Index; BAI, Beck Anxiety Inventory; APPQ, Albany Panic and Phobia Questionnaire; PSWQ, Penn State Worry Questionnaire; LSAS, Liebowitz Social Anxiety Scale; TP, total power; HF norm, normalized high-frequency power; LF/HF ratio, low-frequency power/high-frequency power ratio
Table 3.
PSQI, Pittsburgh Sleep Quality Index; BAI, Beck Anxiety Inventory; APPQ, Albany Panic and Phobia Questionnaire; PSWQ, Penn State Worry Questionnaire; LSAS, Liebowitz Social Anxiety Scale; TP, total power; HF norm, normalized high-frequency power; LF/HF ratio, low-frequency power/high-frequency power ratio







