Disturbance of Sleep and Circadian Rhythm in Hospitalized Patients
Article information
Abstract
Sleep and circadian disturbance are common in hospitalized patients. Problems related to sleep induction, frequent awakening, poor sleep quality, and disturbed circadian rhythm including daytime somnolence and nighttime arousal are frequently observed in the hospital. Disturbance of sleep and circadian rhythm could interfere recovery of the patients, prolong the length of stay, and contribute to patient dissatisfaction. Various factors affect sleep and circadian rhythm disturbance in the hospital. Intrinsic factors are related to patients, including medical and psychiatric conditions, uncontrolled pain, prescribed medications, and physical inactivity. External factors related to the hospital environment such as noisy environment, excessive exposure to artificial light, inappropriate humidity, and temperature are also known interrupters for sleep. Medical care provided by professionals, including nighttime vital sign monitoring, phlebotomy, and medication administration, can also contribute to sleep and circadian rhythm disturbances. This review aims to systematically address sleep and circadian rhythm disturbances in hospitalized patients, discuss factors that affect sleep in the hospital, and suggest non-pharmacological and pharmacological treatment options.
INTRODUCTION
Sleep is essential for human health. It is assumed that sleep is a vital process for memory consolidation, regulation of immune system and neuroendocrine function, cognition, and mood stability [1-3]. Disturbance of sleep could lead to various physical and psychological health problems [4]. It is known that sleep disturbance, including poor sleep quality and short or long sleep duration, is associated with overall mortality [5-8], metabolic syndrome including impaired glucose metabolism or diabetes [9-14], hypertension [14,15], coronary heart disease [16-18], and psychiatric symptoms including depression or anxiety [19-21], or impaired neurobehavioral performances [22-24].
Hospitalized patients are those in need of medical attention, suffering from acute exacerbations of health conditions. Sufficient sleep is what they need to recover from their condition, however, many of them experience sleep disturbance in the hospital. A previous study claimed that the sleep quality of hospitalized patients is similar to that of patients with sleep disorders [25]. In addition, hospitalized patients also report that their subjective sleep quality and quantity are poor compared to habitual sleep at home, as reported by 2,005 hospitalized patients [26]. There is also a high rate of use of sleeping pills in hospitalized patients. Previous studies have shown that approximately 26%–29% of hospitalized patients are prescribed sedative-hypnotics for sleep [25,27]. In critically ill patients, the prevalence of sleep disturbance increases. According to a systematic review of the literature about sleep disturbance in critically ill hospitalized patients, the prevalence of sleep disturbance ranged from 50% to 66.7% within a month after hospitalization [28].
The consequences of sleep disturbance in hospitalized patients are also heavy. Previous literatures have claimed that sleep disturbance can contribute to prolonged length of stay, impaired recovery, and poor patient satisfaction [1,2,29]. Sleep disturbance can impair recovery due to its intrinsic negative health consequences, including impaired immunologic function or metabolic derangement [30,31]. In a study with 212 hospitalized patients, sleep loss in the hospitalized patients was found to be associated with impaired fasting glucose and hyperglycemia [32]. Daytime somnolence and fatigue related to sleep disturbance could hinder therapeutic daytime activity of patients, especially in the elderly population [33,34]. In addition, the development of delirium is also linked to sleep disturbance, which is an important health condition in the hospital [35-37]. Thus, it is important to pay attention to the sleep disturbance of hospitalized patients.
SLEEP AND CIRCADIAN DISTURBANCE IN THE HOSPITAL
Insomnia is a prevalent sleep problem among hospitalized patients, as well as in the general population [2,38]. According to Ho et al. [39], 36% of hospitalized patients in a group of 205 inpatients experienced new-onset insomnia during their hospital stay. Insomnia during hospitalization manifests as difficulty in sleep induction, maintenance, poor sleep quality, fragmented sleep, and sleep deprivation. Adult hospitalized patients experience a sleep time loss of approximately 18%, while pediatric patients experience 20%–25% sleep loss [26,40]. A study on sleep quality and quantity in hospitalized patients (n=2,005) revealed that sleep onset latency (SOL) was 21 minutes shorter compared to their habitual sleep, while their wake after sleep onset (WASO) was 29 minutes longer [26]. They were also found to have shorter sleep times, poor sleep efficiency (SE), and non-refreshing sleep. Studies using polysomnography in acute care units showed that critically ill patients frequently experience fragmented sleep with increased N1 and N2 sleep, decreased duration and frequency of slow wave sleep (SWS), and rapid eye movement (REM) sleep [41,42]. Hospitalization could be also a predisposing factor to the development of chronic insomnia after discharge. According to Griffiths and Peerson [43], 19% of 86 patients developed chronic insomnia within three months after discharge.
Sleep-disordered breathing, such as obstructive sleep apnea (OSA), is a common sleep problem in both pre-existing and newly developed sleep disorders in hospitals [42]. The risk for OSA using the Berlin questionnaire among 424 hospitalized patients was found to be up to 39.5% [44], while the STOP-BANG questionnaire revealed up to 80% of 195 hospitalized patients at risk [45]. In OSA patients, episodes of complete or partial pharyngeal obstruction during sleep are observed, causing snoring or apneic episodes. This could lead to intermittent nocturnal sympathetic activation, resulting in nocturnal hypoxia, frequent awakening, cortical arousals, daytime symptoms of fatigue, sleepiness, and cognitive impairment [3]. Despite its high prevalence and ill consequences, it is assumed that many of OSA patients in the hospital remain undetected [46,47]. Early screening and detection of OSA in hospitalized patients could prevent further ill outcomes of untreated OSA, including cardiovascular disease [48]. Continuous positive airway pressure therapy is recommended as the first-line treatment for OSA in hospitalized patients [49].
The circadian disturbance is another important factor affecting sleep of hospitalized patients. The role of circadian rhythm is not confined to sleep alone. It dictates metabolic, hormonal, and immunologic functions, and modulates molecular machinery [50,51]. The circadian rhythm regulates the inflammatory response, ensuring appropriate timing and maintenance of the immune process, which is an essential process in hospitalized patients [51]. The suprachiasmatic nucleus (SCN) is the pacemaker of circadian rhythm and performs a critical role in controlling and coordinating the activity of circadian oscillators in the body [52,53]. The SCN modulates the secretion of melatonin, which carries time information from the brain to the body [54]. Many external stimuli could entrain the SCN, and among them, light is the most critical factor [55]. Excessive light exposure during the night or insufficient light exposure during the daytime in the hospital could disorganize the circadian system [56,57]. Circadian disturbance could also occur when the sleep and wake schedule of the hospital is different from the chronotype of the individual. A previous study showed that 56% of 117 hospitalized patients reported earlier bed and wake times compared to their habitual sleep schedule as a disruptor of their sleep [58]. The disturbed timing of food is also a risk factor for circadian disturbance [59]. In critically ill patients, interruption of enteral nutrition could disturb circadian rhythm [41]. Additionally, the medical condition of hospitalized patients could alter the circadian rhythm. Systemic inflammation may disrupt circadian rhythm, as a correlation between circadian disruption and inflammatory cytokines in septic patients was found in previous studies [60,61]. Decreased melatonin levels could be found in many disease conditions, including insulin resistance, type 2 diabetes, migraine, cancer, and Alzheimer’s disease [62]. Old age alone is also a risk factor for decreased melatonin levels due to reduced transparency of the lens, which could lead to a higher prevalence of circadian disturbance in elderly hospitalized patients [63].
FACTORS AFFECTING TO SLEEP AND CIRCADIAN RHYTHM DISTURBANCE IN THE HOSPITALIZED PATIENTS
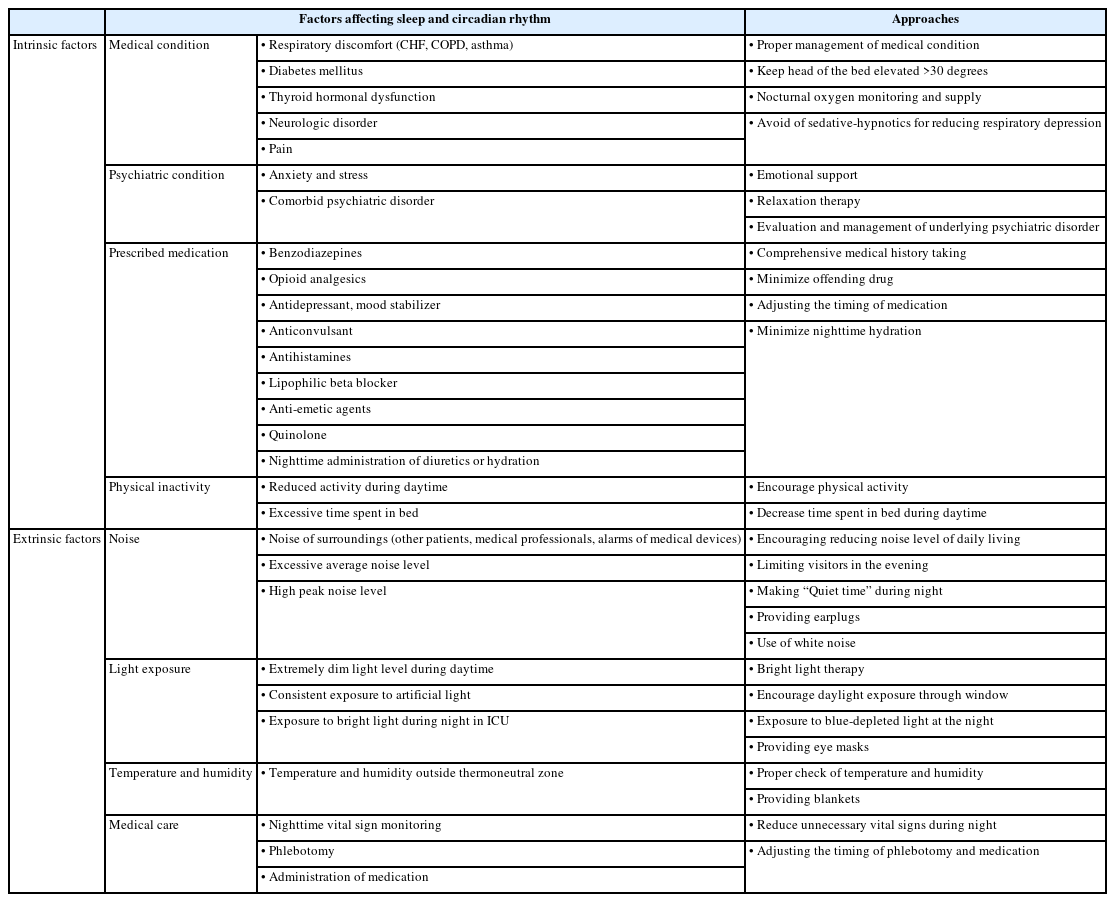
Various factors affect the sleep and circadian rhythm of hospitalized patients, which can be classified as internal and external factors [26,39,64]. Internal factors relate to the patient’s medical condition including pain, psychiatric condition, prescribed medications, and physical inactivity. External factors can be divided into environmental factors, including noise, light exposure, humidity, and temperature of the surroundings, and medical care factors, such as vital sign monitoring, phlebotomy, and nighttime administration of medication (Table 1).
Intrinsic factor
The medical conditions of hospitalized participants themselves could be risk factors for sleep disturbance. Patients with respiratory discomfort, such as congestive heart failure, chronic obstructive pulmonary disease, or asthma, often report frequent nighttime arousals and awakenings, which can lead to sleep deprivation [65]. In particular, respiratory muscles, except the diaphragm, become atonic in REM sleep, and episodes of oxygen desaturation can occur in patients with respiratory discomfort [66]. Metabolic disorders could be also risk factors for sleep disturbance. Patients with diabetes mellitus are known to have decreased total sleep time (TST) and poor sleep quality, possibly due to frequent nocturia and diabetes-related neuropathic pain [67]. Thyroid hormonal dysfunction is another factor associated with sleep disturbance. Patients with hypothyroidism tend to have reduced SWS, poor sleep quality, and daytime somnolence, while patients with hyperthyroidism experience prolonged SOL and disturbed sleep maintenance [42,68]. Neurologic disorders including stroke, epilepsy, neurodegenerative disorders, and traumatic brain injury are also associated with a higher prevalence of sleep disturbance [69]. Pain is another medical condition associated with impaired sleep. Approximately 67% to 88% of patients with chronic pain disorders experience sleep discomfort [70,71], and a study of 772 insomnia patients found that 50% of them suffer from chronic pain [72]. The most common sleep complaint associated with chronic pain is multiple nocturnal awakenings due to pain-related arousals [72]. There is also a reciprocal influence between sleep and pain [73]. Continued sleep disturbance can elevate pain severity in patients, resulting in a prolonged length of stay and patient dissatisfaction [74].
Psychiatric conditions related to hospitalization, such as anxiety and stress, are significant factors related to sleep disturbance. In the hospital, various factors, including the lack of self-control, the feeling of abandonment and insecurity, an unfamiliar environment, and worries about the future or disease, can trigger stress and anxiety [75]. Anxiety and stress could result in sympathetic activation, which could lead to frequent awakening and fragmented sleep [76]. Underlying comorbid psychiatric disorders can also affect sleep. It is estimated that about 65% of individuals with major depressive disorder experience symptoms of insomnia, including frequent awakening, increased SOL and WASO, early morning wake time, decreased TST and SWS, and increased REM sleep [77,78]. Patients with an anxiety disorder also suffer from disrupted sleep continuity, increased SOL, decreased TST, and reduced non-REM sleep [79]. Some researchers claim that insomnia could be a marker for undiagnosed psychiatric disorders [42]. In a study with 200 hospitalized medical patients, patients with insomnia had a 3.6 times higher risk of having major depressive disorder [80].
Many prescribed medications can have an impact on sleep and circadian rhythm. Sedative drugs, such as hypnotics and anxiolytics, as well as opioids, are associated with daytime somnolence, disruption of the circadian rhythm due to daytime napping, and decreased SWS and REM sleep [81,82]. Anticonvulsants and antihistamines are other sedating drugs that could increase daytime somnolence [83,84], and H2 receptor antagonists can be also sedating [42,85]. Antidepressants and mood stabilizers can also alter sleep architecture by decreasing REM sleep [86,87]. Beta-blockers, especially lipophilic drugs, can induce frequent awakenings [88]. Central nervous system agents related to norepinephrine or dopamine are known to reduce SWS and REM sleep [42]. Among antiemetic agents, dopamine antagonists can affect sleep with activating effects [85]. Nighttime diuresis related to the use of diuretics or excessive hydration may lead to sleep disturbances and falls, especially in elderly patients [42,89]. Among antibiotics, quinolones have been reported to cause sleep disturbances [85].
Physical inactivity and excessive time spent in bed are common among hospitalized patients. However, regular physical activity and decreased time spent in bed can improve insomnia symptoms, as recommended in the concept of sleep hygiene [90]. A study involving 25 hospitalized patients found that physical activity and rest based on the circadian rhythm were significantly related to the improved length of stay and functional recovery [91]. Furthermore, many previous studies conducted outside of hospitals have shown that physical activity is associated with better sleep [92-94]. Therefore, physical inactivity and excessive time spent in bed may result in sleep or circadian disruption during hospitalization [95]. However, there is a lack of literature on the association between physical activity and sleep in hospitalized patients, and the results of available studies are controversial. One study on hospitalized patients with dementia reported that increased daytime physical activity was associated with higher sleep duration and efficiency [96], while another study involving 120 hospitalized patients found no significant association between daytime physical activity and sleep [97].
Extrinsic factor
In hospitals, various types of noise including noise from other patients, medical professionals, phone calls, and alarms from medical devices are frequently present. Many hospitalized patients report difficulty sleeping due to noise disturbance [26,98]. Wesselius et al. [26] found that noise is the most disturbing factor to the SOL and the second most disturbing factor to the nocturnal awakening in a study of 2,005 hospitalized patients. Another study examining sleep in the intensive care unit (ICU) found that noise affected 30.8% of arousals in 3,443 patient-days [98]. The noise in the environment can trigger arousal by affecting cortical brain activity and increased heart rate during REM sleep [99]. Previous studies about the exposure to continuous noise greater than 39 dB are associated with frequent awakening, poor sleep quality, and decreased TST and REM sleep [100,101]. The World Health Organization recommends that noise levels should not exceed 30 dB with a maximum peak noise level of 45 dB to avoid negative effects on sleep, yet hospital environments are often much noisier [102]. A previous study examining noise levels in hospitals found that the average noise level in medical units was a mean of 38 dB with a mean peak noise level of 70 dB (comparable to noise levels of a vacuum cleaner) between 11 PM and 7 AM [103]. In the ICU, the average noise level was between 35 dB to 55 dB, with a peak noise over 85 dB between 10 PM and 5 AM [102].
Light exposure in hospitals is an important factor that can impact sleep and circadian rhythm. Daylight is considered the optimal source for the proper functioning of the circadian rhythm, while exposure to artificial blue light during the evening and nighttime can hinder the production of melatonin, leading to delayed circadian rhythm and poor sleep quality. In hospitals, patients are often exposed to unnatural light conditions, such as extremely low daylight exposure or bright artificial light exposure during the night [53,104]. Previous studies have found that the mean luminance in medical units during the daytime is around 100 lux, which is five times dimmer compared to the mean brightness in an office [105]. Conversely, patients in ICU units are exposed to excessive artificial light during the night, with maximal nocturnal luminance levels reaching as high as 1,000 lux to 3,000 lux [106].
Temperature and humidity are two additional factors that affect sleep in hospital environments. Proper temperature regulation is essential to maintain the core body temperature, a vital component of the circadian rhythm [107]. The circadian rhythm of the core body temperature begins to decrease when sleep is initiated until approximately 6 hours after sleep onset and then rises in the morning, whereas the proximal and distal skin temperature rises during sleep [108-110]. Humidity is another factor affecting human thermal comfort and maintaining thermoneutrality. Higher humidity levels lead to higher perceived temperature, and lower humidity levels lead to lower perceived temperature [111]. Optimal bedroom environments have temperatures ranging from 17°C to 28°C and a mean relative humidity between 40% to 60% [107]. Temperature and humidity above or below these optimal conditions increase the frequency of awakenings and decrease REM sleep [112,113]. High humid heat conditions also could increase SOL, and WASO and decrease TST, SE, SWS, and REM sleep [114]. In hospital settings, where patients have limited control over their sleep environment, sleep disturbances may arise due to inappropriate temperature or humidity for individuals.
Medical care, including vital sign monitoring, phlebotomy, or nighttime administration of medication, could be the source of sleep disturbance for inpatients. According to Ho et al. [39], 68% of 205 patients surveyed indicated that staff interruption was the major factor disrupting their sleep. Similarly, a study of 2,005 hospitalized patients found that staff interruption was the primary reason for early awakening in hospitals [26]. In hospital settings, medical care may be overperformed beyond what is necessary. For instance, a study of 54,096 patients found that low-risk medical patients received the same level of overnight vital sign monitoring as high-risk patients [115]. Reducing nighttime interventions could help alleviate sleep disturbance in hospital patients. A previous study suggested that reducing vital sign monitoring and medication administration between 10 PM and 6 AM reduced the use of as-needed sedatives from 32% to 16% among 106 hospitalized patients [116].
MANAGEMENT OF SLEEP AND CIRCADIAN RHYTHM DISTURBANCE IN THE HOSPITALIZED PATIENTS
Non-pharmacological approach
Non-pharmacological approaches should be considered first to avoid possible adverse effects of sedative-hypnotics including falls, delirium, and respiratory depression [117]. These interventions may include adjusting environmental factors, such as reducing noise and adjusting lighting, decreasing unnecessary nighttime medical care, utilizing cognitive-behavioral therapy for insomnia (CBT-I), improving sleep hygiene, and relaxation therapy. Various approaches for adjusting factors affecting sleep and circadian disturbance are summarized in Table 1.
Numerous studies have shown that adjusting external environmental factors related to hospitalization, such as noise and light exposure, can significantly improve the sleep of inpatients. For instance, a study of 749 hospitalized patients in 18 wards in an acute hospital implemented a ward good sleep checklist, which included measures such as noise reduction, nighttime light-off, avoiding unpleasant smells, and providing comfortable temperature and bedding. As a result, 22% of patients reported improved sleep quality [118]. In another study, modifying the care routine by reducing noise, minimizing alarms, administering medication before bedtime, and reducing nighttime vital sign checks or phlebotomy significantly reduced the average and peak noise levels in the ward and improved sleep quality among 60 hospitalized patients [119]. Bright light exposure during the daytime and a decrease in light exposure level at the night could improve sleep. A study of 85,021 hospitalized patients found that exposure to natural daylight through a window was associated with improved patient satisfaction, decreased levels of distress, and improved physical capacity [120]. Another study showed that patients in a blue-depleted evening light environment reported a significant increase in sleep regularity, a stabilized sleep-wake cycle, and improved TST and REM sleep [53]. Daytime bright light therapy has also been shown to have a positive effect on hospitalized patients. A previous study that exposed 24 hospitalized patients to 3,000 lux to 5,000 lux of light between 9 AM and 11 AM for four weeks showed an improvement in TST [121]. Another study offered 3,000 lux of light exposure between 9 AM and 11 AM daily for four weeks to 27 dementia patients, resulting in an increase in the percentage of nighttime spent sleeping by 5% and a decrease in the number of awakenings [122]. The provision of protective devices, such as eye masks or earplugs, can also be an effective solution for problems related to noise and light. One study with 88 hospitalized patients found that the use of earplugs improved the subjective experience of sleep [123], while another study with 46 hospitalized patients reported that protective devices prevented a decrease in sleep quality [124].
CBT-I is a known effective therapy for insomnia and is recommended as the first-line therapy for insomnia by the American Academy of Sleep Medicine (AASM) [125]. It consists of cognitive therapy that targets cognitive distortion toward sleep, behavioral therapy including stimulus control and sleep restriction, and sleep hygiene education [125]. Although CBT-I is usually performed for 4 to 6 weeks, a single session of CBT-I can also affect reducing sleep disturbance [126]. Previous studies have demonstrated the effectiveness of CBT-I in medically-ill patients or for hospitalized patients in the psychiatric unit [127-129]. However, implementing CBT-I for general hospitalized patients can be challenging due to the patient’s medical conditions or the limitations of resources and capacity of medical professionals.
Improving sleep hygiene for hospitalized patients can be more easily implemented than a full session of CBT-I and has been shown to have positive effects on sleep [90]. Sleep hygiene for hospitalized patients can include maintaining regular sleep and wake schedule, increasing daytime physical activity, reducing time in bed, avoiding daytime naps, and avoiding caffeine and smoking. Previous literature has attempted to adapt sleep hygiene practices for inpatients. For example, Edinger et al. [130] performed a sleep hygiene protocol, which included reducing daytime napping and standardizing sleep and wake schedules for 321 inpatients, resulting in a 5% increase in TST compared to usual care. Another recent study of 931 patients using sleep hygiene promotion, including a relaxing environment and music, non-caffeinated tea, and a sleep package with eye masks and earplugs, reported an increase in Richards-Campbell Sleep Questionnaire scores [131].
Relaxation therapy, aimed at reducing anxiety, can have a positive impact on sleep quality. Supportive care for relaxation, which includes the use of warm blankets, warm milk, emotional support, and noise reduction techniques, has been shown to reduce SOL among 32 hospitalized patients [1]. McDowell et al. [117] offered 111 patients the choice of all or portions of a three-part intervention, consisting of a back massage, herbal tea or milk, and relaxing music or nature sounds. They found that improved sleep quality and reduced use of hypnotics were significantly correlated with the number of intervention parts received. In a study of 28 hospitalized patients in the ICU, Su et al. [132] demonstrated that soothing music could help to lengthen N3 sleep and improve sleep quality. Another study also reported that earplug-delivered sleep-inducing music before bedtime significantly improved sleep quality and quality in 58 hospitalized patients [133].
Pharmacological approach
Pharmacological therapy may be considered to control sleep or circadian rhythm in hospitalized patients, taking into account the potential risks and benefits. A comprehensive evaluation, including a patient’s history of sleep complaints, medical and psychiatric history, and current medication use, should be performed to determine the most suitable treatment. Factors such as drug efficacy, mechanism of action, and side effect profiles should also be considered [134,135]. US Food and Drug Administration (FDA)-approved drugs for insomnia include benzodiazepines (triazolam, estazolam, temazepam, quazepam, flurazepam), non-benzodiazepines (zolpidem, zaleplon, eszopiclon), melatonin agonist (ramelteon), orexin receptor antagonists (suvorexant, remborexant, daridorexant), and tricyclic antidepressant (doxepin) [136,137]. Sedating antidepressants, atypical antipsychotics, and antihistamines may also be administered off-label to manage sleep [136].
Benzodiazepines are the most commonly used drugs for sleep disturbance. They have been found to decrease SOL and increase TST, as well as provide anxiety-relieving effects [81,138]. However, benzodiazepines have several side effects, including daytime sedation, the potential for tolerance or dependence, rebound insomnia, respiratory depression, and an increased risk of falls, delirium, or cognitive decline in the elderly population [139,140]. Benzodiazepines with short half-lives carry a higher risk for falls, tolerance, and rebound insomnia, while long half-lives may be more associated with daytime sedation, respiratory depression, an increased risk of falls during the night, cognitive decline, or delirium [135,141]. Benzodiazepines should only be administered for short-term use to avoid tolerance, and their use should be avoided in elderly patients due to their increased potential for adverse effects in this population [142,143]. According to the AASM clinical practice guideline, triazolam is recommended for sleep onset insomnia, and temazepam is suggested for both sleep onset and maintenance insomnia [134].
Non-benzodiazepines, also known as Z-drugs, were developed to minimize the adverse effects of benzodiazepines and are selectively targeted to sleep without anxiolytic effects [144]. Meta-analyses of 13 studies have shown that the use of Z-drugs is significantly associated with a reduction in subjective and objective SOL [145]. Z-drugs are known to have less daytime sedation, tolerance or withdrawal potential, and anterograde amnesia compared to benzodiazepine [146-148]. However, Z-drugs also have adverse effects including drowsiness, nausea, dizziness, and unpleasant taste particularly for eszopiclone [148-150]. The use of zolpidem and eszopiclone for sleep onset and maintenance and zaleplon for sleep onset insomnia is recommended by AASM guidelines [134].
Ramelteon, the only FDA-approved melatonin-receptor agonist, targets melatonin 1 and 2 receptors located in the SCN, which may result in stabilized circadian rhythms and sleep-wake cycle [62]. Ramelteon is effective for sleep induction, as proven by its effect in reducing subjective or polysomnographic SOL [151,152]. Due to its mechanism, melatonin agonists do not have adverse effects related to falls, abuse potential, or cognitive decline [151,153]. The most common side effect of ramelteon is dizziness, nausea, and fatigue [153]. The AASM guideline suggests that clinicians use ramelteon for sleep onset insomnia [134].
Orexin receptor antagonists selectively bind to orexin 1 and 2 receptors, which regulate wakefulness and sleep [154]. Suvorexant has been proven to be effective in improving TST and decreasing SOL [155,156]. Considering the clinical trial data and drug mechanism, the potential for abuse or other adverse effects are assumed to be lower in orexin receptor agonists than in benzodiazepines [136]. The most common side effect of suvorexant is somnolence [154]. The AASM guideline suggests the use of suvorexant for sleep maintenance for insomnia [134].
Doxepin is the only FDA-approved tricyclic antidepressant (TCA) for insomnia with sleep maintenance difficulty with a high affinity for histamine receptors [136]. Previous literature reports have shown that the use of doxepin is related to improved TST and decreased WASO and awakenings [157,158]. Due to the lower doses approved for sleep as compared to higher doses used for depression, doxepin has relatively fewer adverse effects [136]. The most common adverse effects of doxepin are nausea and somnolence [159]. According to the AASM guidelines, doxepin is suggested for use in sleep maintenance for insomnia [134].
Sedating antidepressants including trazodone, mirtazapine, or TCA other than doxepin are often used for sleep disturbance in hospitalized patients. While trazodone is an FDA-approved drug for depression, prescription data has indicated that it is more commonly prescribed for insomnia. Lower doses of trazodone are typically recommended for sleep due to a higher risk of anticholinergic adverse effects, including the risk of falls or delirium [160]. A previous study on trazodone use reported a decrease in SOL and WASO in the treatment group compared to the placebo group [161]. However, due to the lack of clinical significance and evidence, the AASM guidelines recommend against the use of trazodone as a treatment for insomnia [134]. Mirtazapine is classified as a noradrenergic and specific serotonergic antidepressant, which causes inverse dose-dependent sedation. The higher dose of mirtazapine is not beneficial for sedation [162]. A previous study found that mirtazapine improved sleep continuity, SE, and SWS compared to a placebo in healthy volunteers [163]. However, there is a lack of research regarding mirtazapine use for sleep disruption in hospitalized patients. Other sedating TCAs, including amitriptyline, nortriptyline, and imipramine, have been utilized for insomnia. However, the use of these drugs is not recommended for sleep disruption in hospitalized patients due to the risk of anticholinergic effects, orthostatic hypotension, and slowed cardiac conduction [135].
Atypical antipsychotics, such as quetiapine, olanzapine, or risperidone, are also often used for sleep disturbance in hospitalized patients. Sedating effects of atypical antipsychotics are associated with their antagonistic effects on serotonin or histamine receptors [164]. For patients with delirium or dementia experiencing sleep disturbance, antipsychotics can be helpful for symptom control [165,166]. However, the use of atypical antipsychotics should be approached with caution due to their adverse effects, including extrapyramidal syndrome, QTc prolongation, anticholinergic effects, hyperglycemia, dyslipidemia, and weight gain [167]. Additionally, there is a lack of evidence regarding the use of atypical antipsychotics for insomnia [168].
Antihistamines are the most commonly used over-the-counter agents for insomnia [169]. However, studies have indicated that they are minimally effective in inducing sleep and may even reduce sleep quality while increasing residual somnolence. Moreover, H1 antihistamines are known to cause rapid tolerance of their sedative effects within a few days of administration, which limits their potential use as sedatives [170]. In addition, antihistamines have potent anticholinergic effects that can cause delirium in elderly hospitalized patients [171]. Therefore, it is recommended to avoid prescribing antihistamines for sleep or circadian disturbance, which is also suggested by the AASM guideline [134].
CONCLUSION
Sleep and circadian rhythm disturbance are common issues faced by hospitalized patients, which can have negative impacts on patient recovery and satisfaction. It is important to identify and address intrinsic and extrinsic factors that contribute to sleep disturbance to improve patient outcomes. Non-pharmacological interventions such as sleep hygiene education, optimizing the hospital environment, and relaxation therapy have been found to be effective in improving sleep. Pharmacological interventions such as hypnotics and sedatives may be necessary for certain situations but should be used judiciously due to potentially adverse effects. Healthcare professionals should also be mindful of the impact of medical care interventions on patient sleep and take steps to minimize their impact. We suggest that clinicians take a systematic approach to managing sleep and circadian disturbance of the hospitalized patients by understanding the major factors affecting sleep and proper treatment options.
Notes
Funding Statement
None
The authors have no potential conflicts of interest to disclose.
Availability of Data and Material
Data sharing is not applicable to this article as no datasets were generated or analyzed during the study.
Author Contributions
Conceptualization: Kyung mee Park. Investigation: Kyung mee Park. Methodology: Kyung mee Park. Project administration: Kyung mee Park. Supervision: Taeyoung Kyong. Writing—original draft: Kyung mee Park. Writing—review & editing: Kyung mee Park, Taeyoung Kyong.