 |
 |
- Search
| Chronobiol Med > Volume 5(4); 2023 > Article |
|
Abstract
Objective
Methods
Results
NOTES
Conflicts of Interest
Availability of Data and Material
The datasets generated or analyzed during the study are available from the corresponding author on reasonable request.
Author Contributions
Conceptualization: Devina Carolina Mastari, Junita Maja Pertiwi. Formal analysis: Devina Carolina Mastari, Windy Mariane Virenia Wariki. Investigation: Ansye Momole, Herlyani Khosama. Methodology: Devina Carolina Mastari, Windy Mariane Virenia Wariki. Software: Devina Carolina Mastari, Windy Mariane Virenia Wariki. Supervision: Finny Warouw, Junita Maja Pertiwi. Validation: Finny Warouw, Junita Maja Pertiwi. Writing—original draft: Devina Carolina Mastari, Windy Mariane Virenia Wariki. Writing—review & editing: all authors.
Acknowledgments
Figure 1.
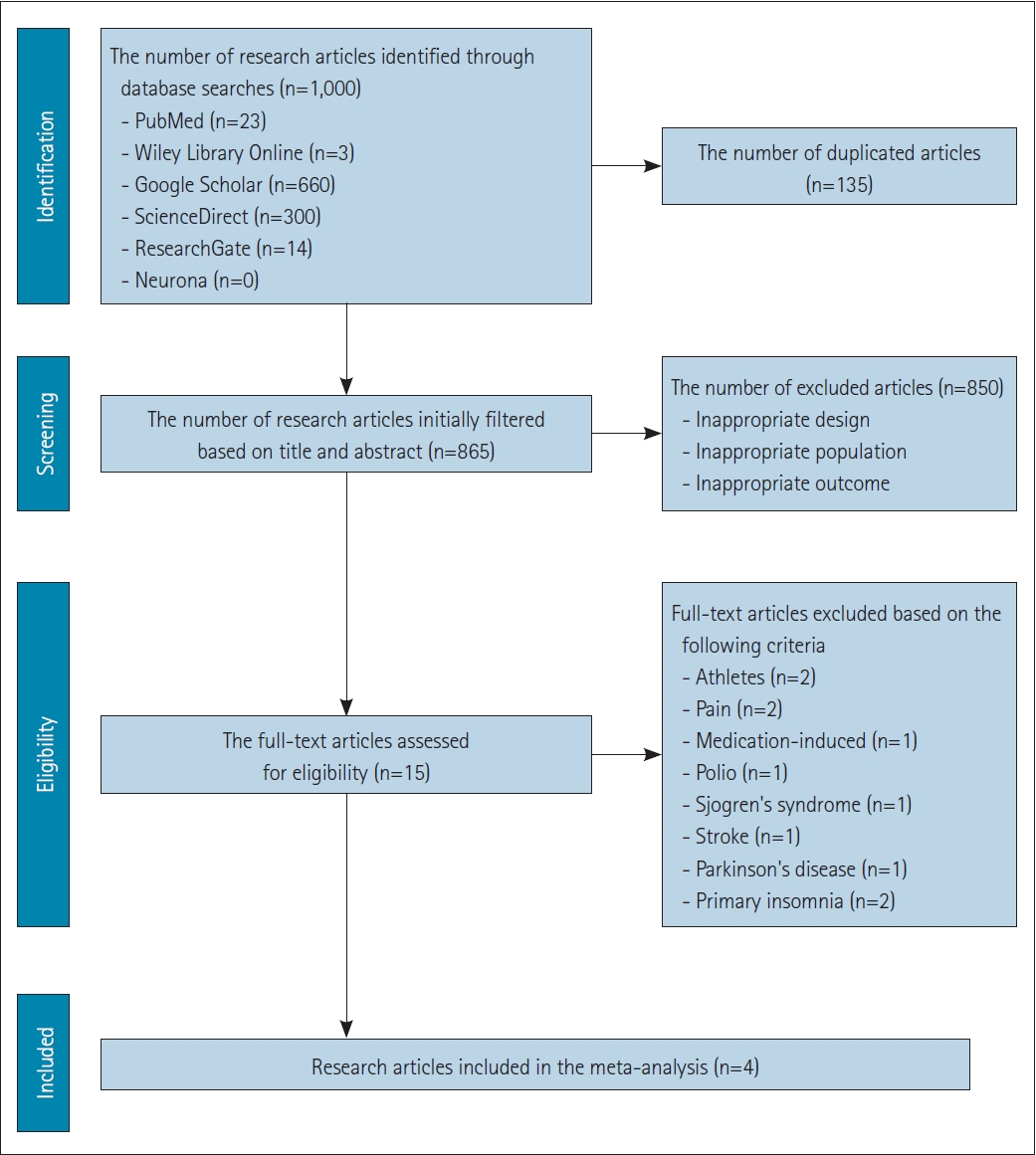
Figure 2.
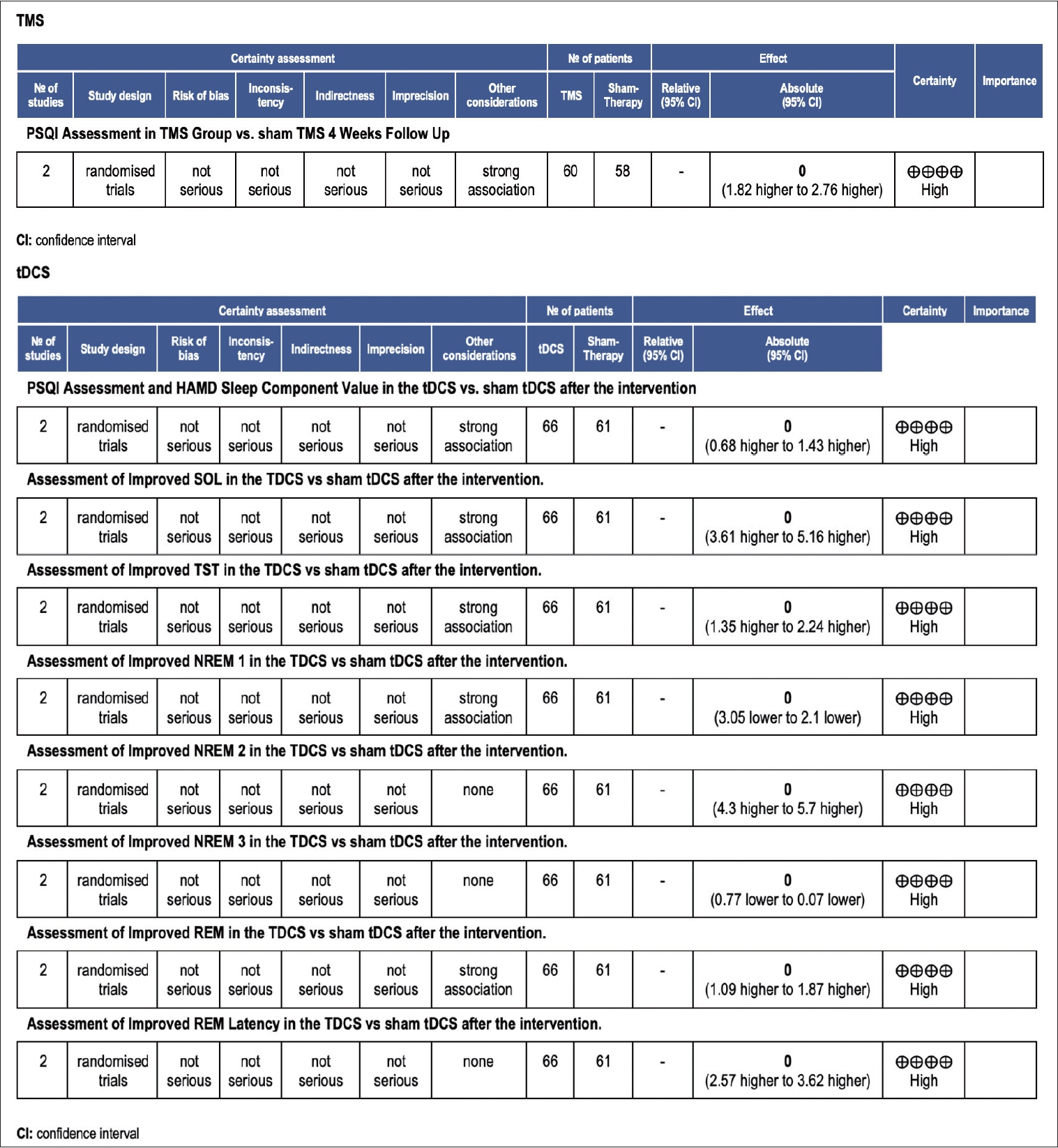
Figure 3.
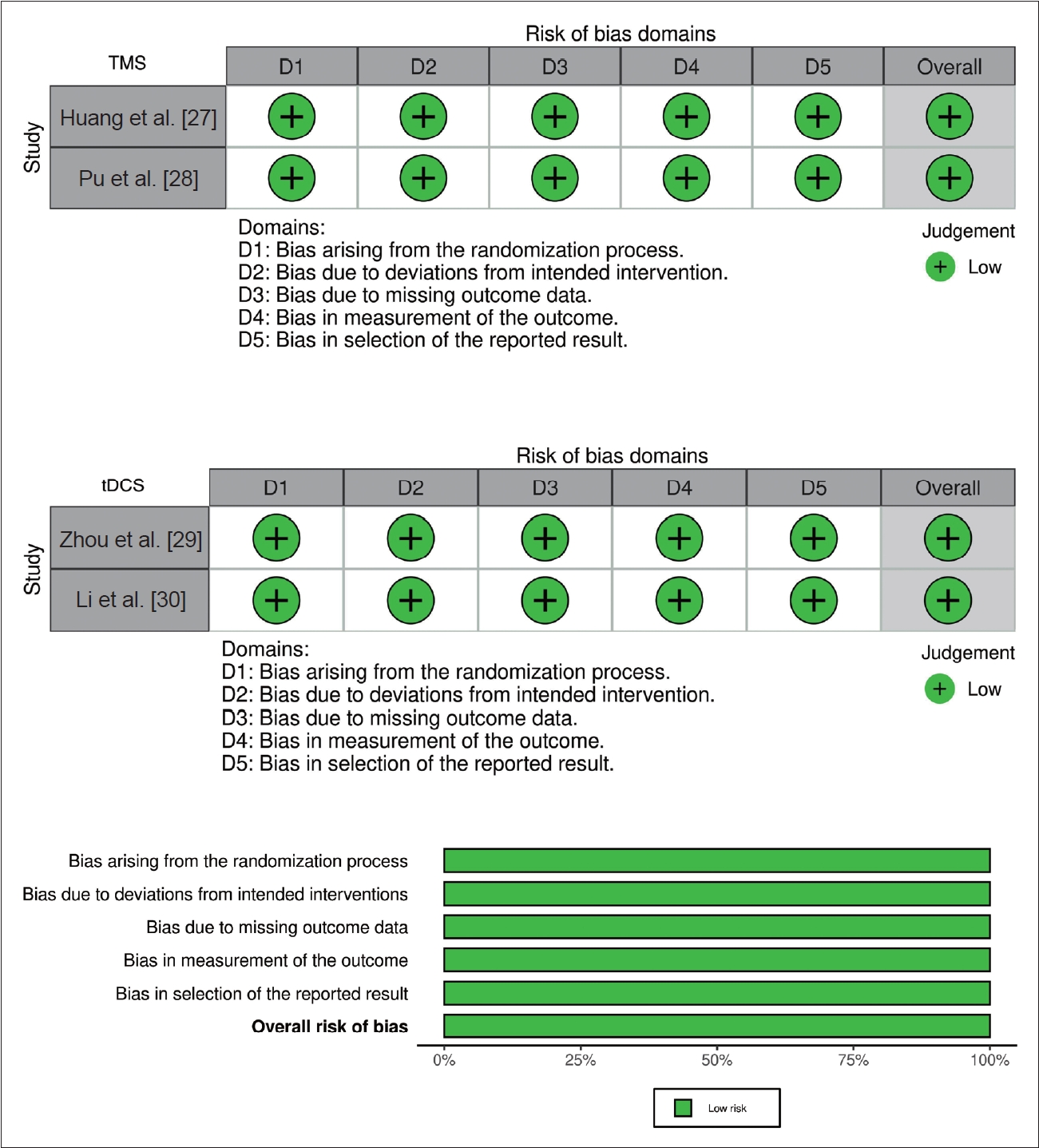
Figure 4.

Figure 5.
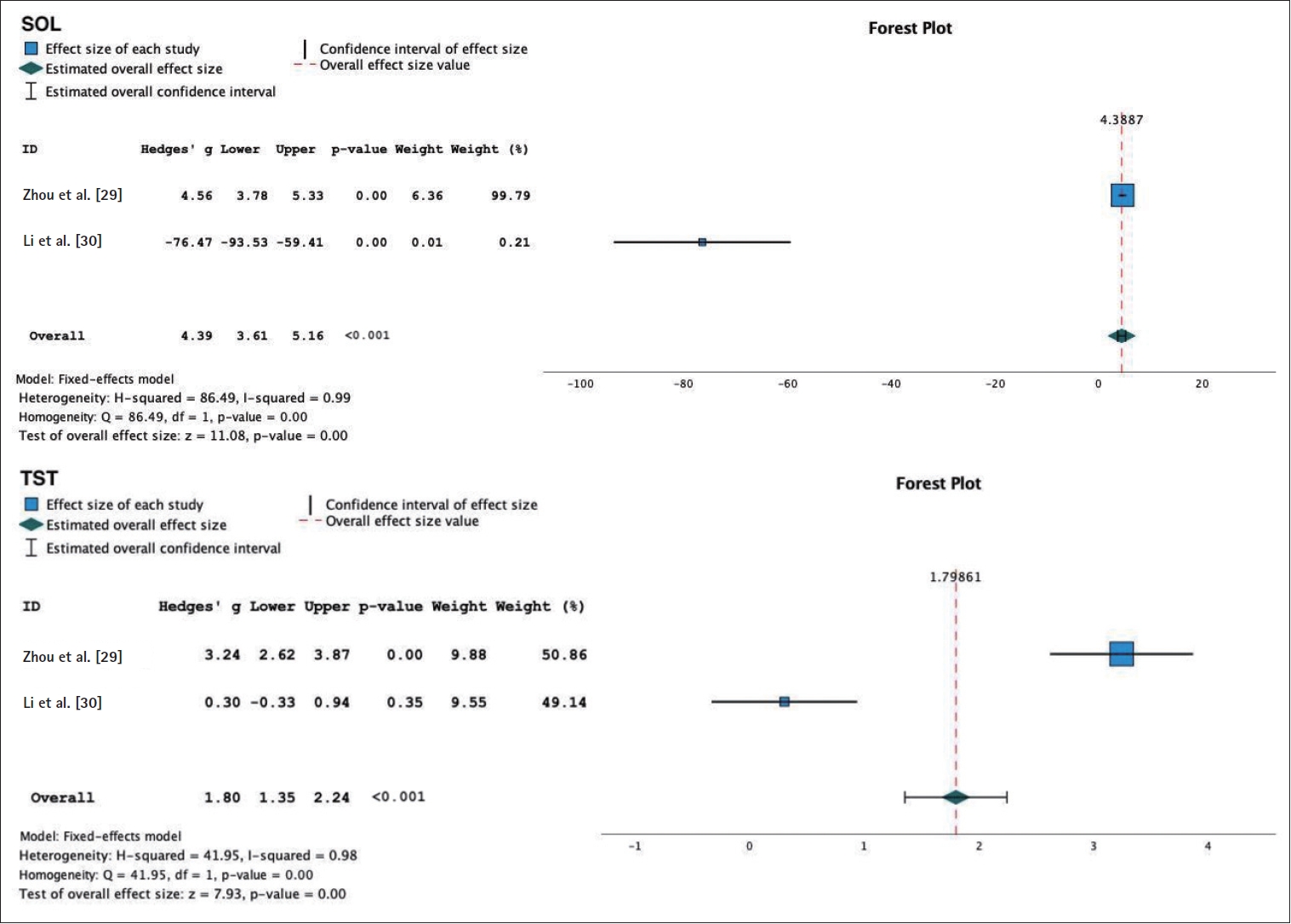
Figure 6.
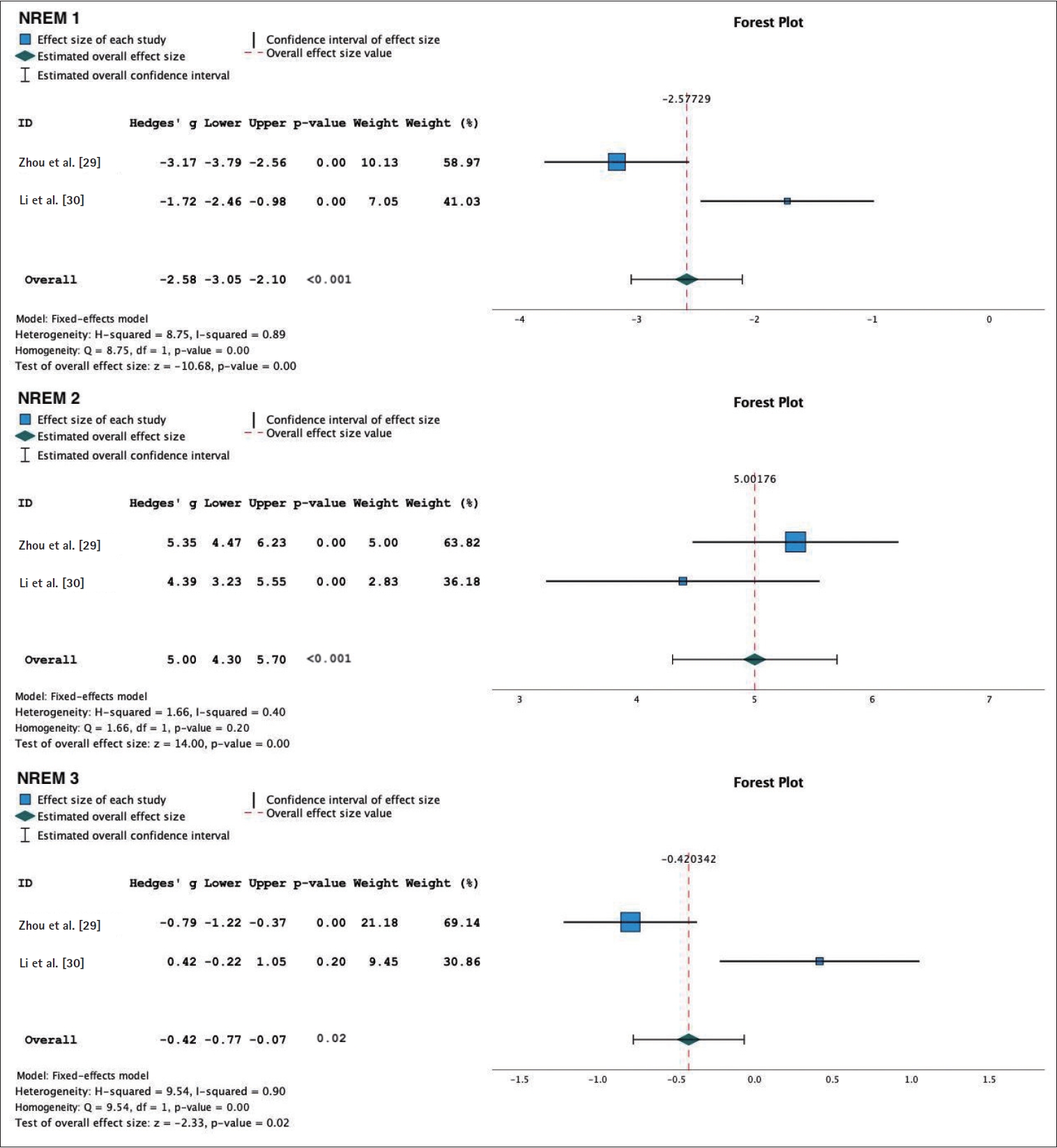
Figure 7.
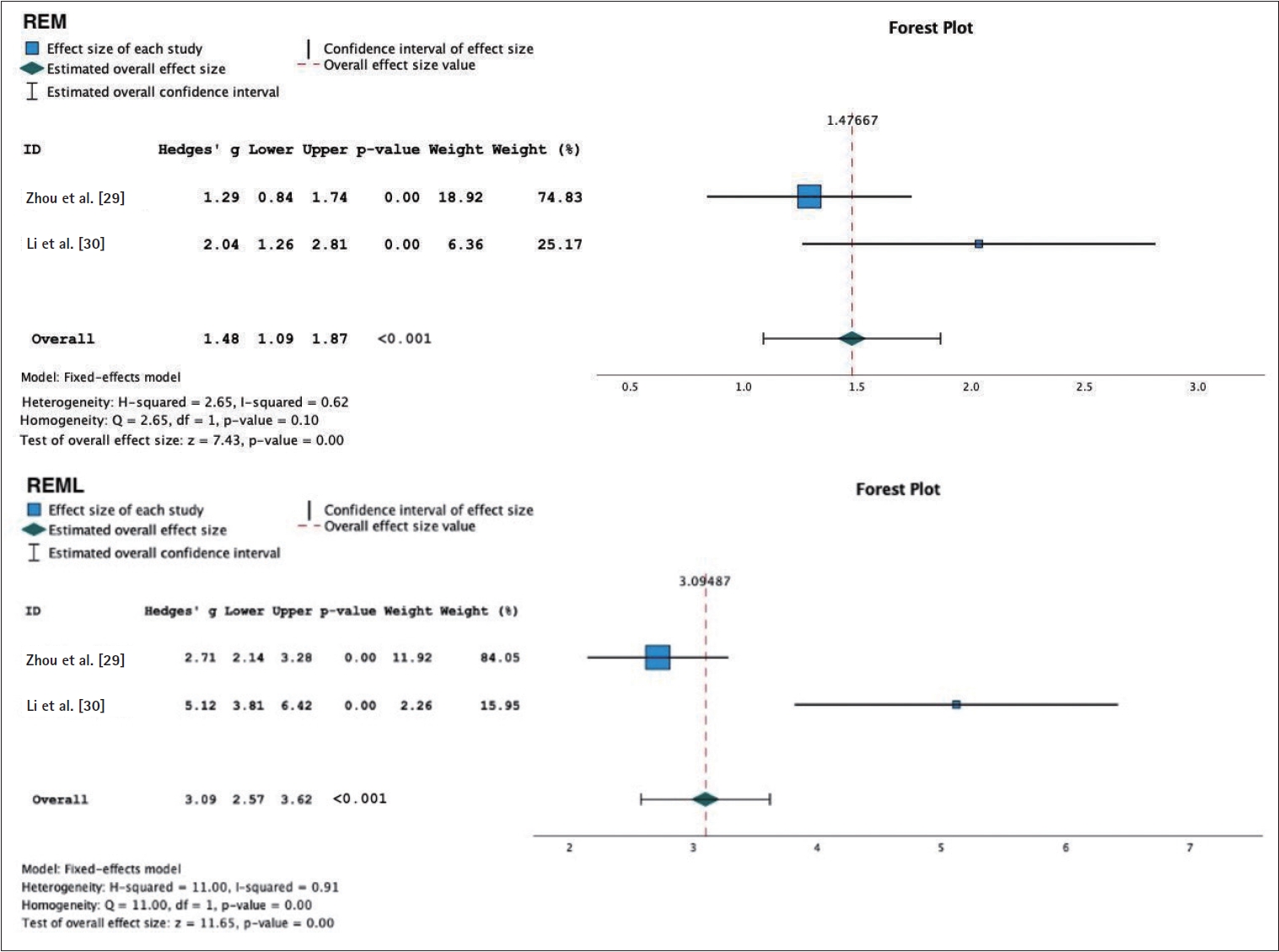
Table 1.
| Study | Age (yr) |
Sample size |
Insomnia diagnosis | Intervention | Comparison |
Location and stimulation parameters |
Duration | Outcome parameters | Outcome results | |||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Total | Active | Sham | Active | Sham | ||||||||
| TMS | ||||||||||||
| Huang et al. [27] | 18–65 | 36 | 18 | 18 | DSM-IV | rTMS+SSRI | Sham+SSRI | Right parietal posterior P4, 1 Hz freqeuency, 90% of motor threshold, 3 trains 500 pulses, interval intertrain 10 minutes | The same as in the active group without magnetic waves | 1 day per session, a total of 10 days (2 weeks) | PSQI | Improvement of insomnia after intervention (week 2), week 4, and week 8 |
| Pu et al. [28] | ≥18 | 82 | 42 | 40 | ICD-10 | rTMS+agomelatine | Sham+agomelatine | Left DLPFC, 10 Hz frequency, 120% of motor threshold, 25 trains of 8 seconds, intertrain interval of 26 seconds | The same as in the active group without magnetic waves | 1 day per session, a total 20 days (4 weeks) | PSQI | PSQI: Improvement of insomnia after intervention (week 4), and week 8 |
| PSG: TST, SE, SOL, WASO, MAT, N1, N2, N3, REM | PSG: Increase of TST, SE, N3; Reduction of SOL, N1 | |||||||||||
| tDCS | ||||||||||||
| Zhou et al. [29] | 18–65 | 90 | 47 | 43 | ICD-10 | tDCS+escitalopram+zoplicone | Sham+escitalopram+zoplicone | Anode: left DLPFC, cathode: right DLPFC, 2 mA intensity | The same as in the active group, the stimulation is applied for 30 seconds and then stopped | 1 day per session, a total 20 days (4 weeks) | PSQI | PSQI: Improvement of insomnia |
| PSG: SOL, TST, SE, AHI, REML, REM, N1, N2, N3 | PSG: Increase of TST, SE, REML; Reduction of SOL, AHI | |||||||||||
| Li et al. [30] | 20–65 | 37 | 19 | 18 | PSG | Escitalopram/duloxetine for 2 weeks → tDCS | Escitalopram/duloxetine for 2 weeks → Sham | Anode: F3, cathode: F4, 2 mA intensity | The same as in the active group, the stimulation is applied for 10 seconds and then stopped | 1 day per session, a total 10 days (2 weeks) | PSG: SOL, TST, AHI, REML, REM, N1, N2, N3 | PSG: There was no significant changes |
| The HAMD insomnia component | The HAMD insomnia component: Improvement of insomnia after intervention | |||||||||||
TMS, transcranial magnetic stimulation; tDCS, transcranial direct current stimulation; DSM-IV, Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition; SSRI, selective serotonin reuptake inhibitors; PSQI, Pittsburgh Sleep Quality Index; ICD-10, International Classification of Disease, 10th Revision; DLPFC, dorsolateral prefrontal cortex; PSG, polysomnography; TST, total sleep time; SE, sleep efficiency; SOL, sleep onset latency; WASO, wake after sleep onset; REM, rapid eye movement; AHI, apnea-hypopnea index; REML, rapid eye movement latency; MAT, micro-awakening times; HAMD, Hamilton Depression Rating Scale
Table 2.
| Group |
Outcome |
Z | p | |
|---|---|---|---|---|
| Mean rank | Sum of ranks | |||
| TMS (n=2) | 3.50 | 7.00 | -1.549 | 0.121* |
| tDCS (n=2) | 1.50 | 3.00 | ||







