Circadian Misalignment and Bipolar Disorder
Article information
Abstract
The circadian rhythm is a periodic and continuous change caused by the light/dark cycle as the Earth rotates around its own axis in a 24- hour cycle. The circadian clock system regulates the 24-hour daily rhythms of human physiology and behavior such as the sleep/wake cycle, body temperature, hormone secretion, and mood. The influence of circadian rhythm on the body and mind is obvious, but considerable research has not dealt with its effects on human disease, especially on mental illnesses. However, several recent studies have shown that circadian misalignment may play an important role in the pathogenesis of bipolar disorder. Evidence for circadian rhythm misalignment in bipolar disorder suggests that circadian rhythm phase shift is a key pathophysiologic mechanism.
INTRODUCTION
The relationship between bipolar disorder and circadian rhythm has long been considered. Kraepelin [1] mentioned the link between mental illnesses and sleep disturbance in his book and most psychiatrists clinically observe that disturbance of the sleep-wake cycle is closely related to the recurrence of bipolar disorders. Sleep loss is often observed in manic episodes, and insomnia or hypersomnia is common in depressed episodes [2]. There is evidence that patients with bipolar disorder have sleep problems even in euthymic status [3]. However, sleep is only one aspect of the circadian rhythm. The circadian rhythm is a large and basic phenomenon.
Circadian rhythm is a phenomenon caused by the cycle of light and dark, as the Earth rotates around its own axis in a 24-hour cycle. The Earth’s day and night cycle has influenced life since its origin billions of years ago; all creatures on Earth have evolved with a circadian rhythm in their physiology and behaviors. Circadian rhythm works at a genetic level in all living creatures. The Nobel Prize for physiology and medicine in 2017 was awarded to the researchers Jeffrey C. Hall, Michael Rosbash, and Michael W. Young who discovered the role of clock genes in Drosophila [4]. In humans too, the circadian rhythm is pervasive in various physiological functions and behaviors, such as the sleep-wake cycle, body temperature, hormonal secretion, cognitive function, and mood changes [5]. Mood disorder has been reported to be associated with circadian rhythm disturbance, especially in bipolar disorder [2,6-8]. This review focuses on the evidence that circadian rhythm misalignment in bipolar disorder may be a key pathophysiological mechanism and discusses the possible clinical implications.
WHY DOES CIRCADIAN RHYTHM MISALIGNMENT OCCUR?
Humans have survived by adapting to the 24-hour circadian cycle. Surprisingly, humans have a biological rhythm that is longer than 24 hours. Nevertheless, we live in a 24-hour cycle because of the morning light exposure. The circadian rhythm is shifted a little earlier every morning and set for a 24-hour cycle. In mammals, when a light stimulus enters the retina of the eye, the axons of the retinal ganglion cells transmit signals to the suprachiasmatic nuclei (SCN). The SCN is located in the anterior hypothalamus above the optic chiasm, which is the master pacemaker of the mammalian circadian rhythm [9]. In animal experiments, when the SCN was destroyed, the circadian rhythm was disrupted, but returned to normal when transplanted with SCN cells [10,11].
The SCN regulates the circadian rhythm of the body through the endocrine system and the nervous system pathways. Signals from the SCN are transmitted to the hypothalamic neurons and various parts of the brain to produce diverse circadian rhythms such as the sleep cycle, body temperature regulation, and hormone secretions [12,13]. The SCN maintains control across the body by synchronizing oscillators, which exhibit their own near24-hour rhythm and control circadian phenomena in the local tissues [14]. The intrinsic circadian rhythm controlled by this process is associated with the solar day-night cycle.
The phase response curve (PRC) is a curve that describes the relationship between the timing of the light exposure and the circadian phase shift. This curve shows that the changing patterns of sleep-wake cycle, fluctuations in hormonal secretion, mood variations, and other physiological rhythms are shifted, advanced, or delayed according to the timing of light exposure. Because the most powerful external factor that affects the circadian rhythm shift is bright light, PRC shows the phase shift according to bright light exposure [15]. PRC also indicates how the circadian rhythm is controlled naturally during seasonal changes in the length of the day, alteration of the circadian rhythm by shift work, and jetlag. It also shows when light exposure should be carried out to artificially advance or delay the circadian rhythm. Figure 1 shows the phase shift of the circadian rhythm based on an experiment in which there was exposure to 3,000 lux of white light for 3 hours on 3 days [16].
The degree of circadian phase shift due to light exposure depends on a variety of factors, such as the time of light exposure, how bright the light is, the duration of exposure, the color of light, the individual’s characteristics, etc. As shown in Figure 1, the intersection point where the circadian rhythm is delayed or advanced is around the core body temperature minimum, either before or after it occurs. This crossing is normally around 04:00, 2 hours before awakening, but can vary according to the season and the individual’s condition.
The human circadian rhythm, which is longer than 24 hours, is advanced by dozens of minutes every morning because light exposure is normally placed at the end of the PRC’s advance zone. If an individual does not receive enough light all winter and sleeps and wakes up late, there is circadian delay which makes it difficult to normalize the circadian rhythm. Therefore, people suffer from the so-called “spring fever” in early spring. In this day and age, it is common for many people to stay indoors during the day, so there is insufficient light exposure to maintain the 24-hour rhythm. In modern society, people use excessive artificial lighting at night. Particularly, bright light exposure during bedtime delays the circadian rhythm (Figure 1). In addition, with the advent of tablet personal computers and smartphones, there is direct exposure to intense light late in the night. Long-term use of these devices at night can delay the circadian rhythm easily.
CIRCADIAN MISALIGNMENT IN BIPOLAR DISORDER
Evidence for the association between circadian misalignment and bipolar disorder is accumulating. There is considerable research on the relationship between diurnal rhythm variation and mood episodes in bipolar disorder, and it has been reported that sleep-wake cycle abnormality precedes mood fluctuations in bipolar disorder [17]. The irregularity of the sleep-wake cycle worsens the manic/depressive symptoms, which can be easily understood empirically. The sleep-wake cycle is a part of the circadian rhythm and studies have determined that circadian rhythm misalignment is a biomarker in mood episodes. In a study conducted by my group, circadian rhythms in bipolar disorder were evaluated at admission, at 2-week intervals during hospitalization, and at the time of discharge. All participants wore wrist actigraphs during the study. Saliva and buccal cells were obtained at 8:00, 11:00, 15:00, 19:00, and 23:00 time points, for two consecutive days. Samples of saliva and buccal cells were used for analysis of cortisol and circadian rhythm genes, respectively [18]. This study suggests that acute mood episodes are related to circadian rhythm misalignment between the individual’s endogenous circadian rhythms and his or her physical environment. Acute manic episodes were usually associated with endogenous circadian rhythm acrophases averaging 7-hour advanced (earlier) than those of controls, though these acrophases could have resulted from an average of 17-hour clockwise delays. Mixed manias were 6-hour phase delays, whereas depression was associated with 4–5 hour phase delays compared to the controls. The phase shift of this circadian rhythm was normalized just before discharge. The length of hospital stay varied from two weeks to three months [18]. Based on these results, Figure 2 shows the circadian rhythm phase shift according to episodes of mood disorders. This illustration will explain how the circadian phase shifting relates to changes in mood symptoms.
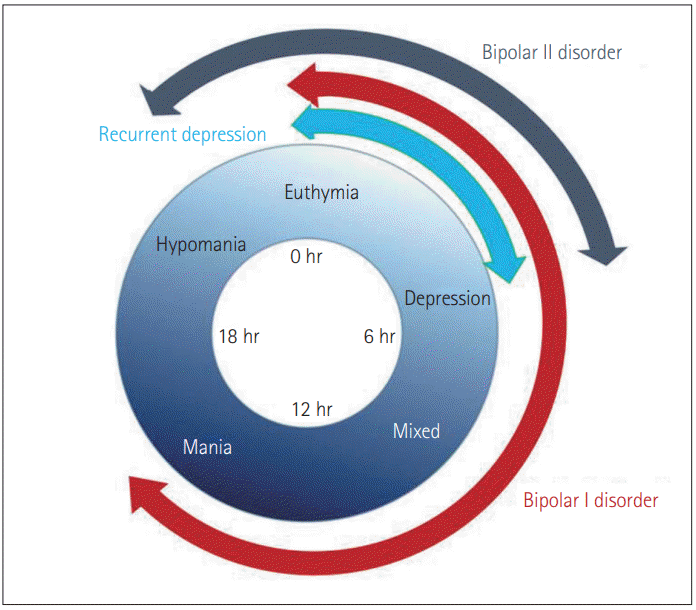
Circadian rhythm shifting vulnerability and mood disorder. The pathogenesis of both recurrent depression and bipolar disorder is related to circadian rhythm shifting tendency. Recurrent depression shows vulnerability of shifting between normal acrophase and 5–6 hr delay. Bipolar II disorder shows advanced shifting between 3–4 hr and 5–6 hr delay, while bipolar I disorder shows the shifting between the normal acrophase and ~16 hr delay.
The circadian phase shift hypothesis of mood episodes is based on the fact that mood episodes last for a relatively long time. It takes more than two weeks to recover from mood episodes, which is similar to the recovery from jet lag. The increase in synaptic neurotransmitters in the brain by antidepressants occurs within several hours after drug administration, but the antidepressant effect usually becomes apparent only after two weeks. This may be due to the time required to normalize the whole-body circadian rhythm, which is the reason why antidepressants have a delayed therapeutic response. Recently, three antidepressant modalities have become the focus of research because of their very rapid antidepressant effect: sleep deprivation, electroconvulsive therapy, and ketamine therapy [19-21]. Previous evidence suggests that the mechanism underlying the antidepressant effect is a process in which the delayed circadian rhythm is restored to normal by treatment [22].
MIXED FEATURE AND MANIC SWITCH
The development of a mixed feature in which mania and depression appear at the same time, is a very difficult phenomenon to explain. The manic switch, which involves rapid changes from depression to a sudden manic episode is also difficult to explain.
Figure 2 is useful in understanding the pathological physiology of mixed features from a circadian rhythm perspective. The circadian phase of the mixed feature is a transitional state in which there is more delay than that of depression and less delay than that of mania. It explains why the mixed feature is unstable and cannot be sustained. The circadian phase of the manic episode seems to be more advanced, but while there is a question whether it is advanced or extremely delayed, the final result is the same in both. I believe that it is the result of extreme delay. The delay of the circadian rhythm occurs relatively easily, but it is very difficult for the advancing phenomenon to occur. In addition, the fact that depression usually appears before the manic episodes supports this assumption.
The manic switch, which is the abrupt development of a manic episode right after a depressive episode, can be explained by the circadian rhythm model shown in Figure 2. Excessive light exposure at inappropriate times due to an irregular daily life rhythm can result in drastic changes in the circadian phase, which can manifest as a manic switch.
SPRING PEAK OF SUICIDE AND MANIA
Previous studies have reported that manic episodes in bipolar disorder and suicides peak during spring. It has been suggested that the sudden increase in the duration and amount of sunlight is a possible cause of these phenomena [23,24]. The increase in mania and suicide in spring can be well explained according to the circadian rhythm model suggested in a previous report [25].
Figure 3 illustrates why mania and suicide are prevalent in spring. Circadian phase delays usually happen due to insufficient light exposure in the morning along with inappropriate light exposure at midnight. During winter, the circadian phase tends to be delayed because of late sunrise. A depressed patient has a more delayed circadian phase in winter compared to a normal person. During spring, the circadian phase of a normal person advances according to an earlier time of sunrise. On the contrary, a depressed patient in winter who has a more delayed endogenous circadian phase further delays his/her circadian phase during spring, since his/her bright light exposure occurs during the “delay zone” of the PRC for light as seen in Figure 3. This significantly delayed circadian rhythm is then able to induce mixed/manic episodes or emotional instability, leading to a possible suicide attempt in susceptible individuals.
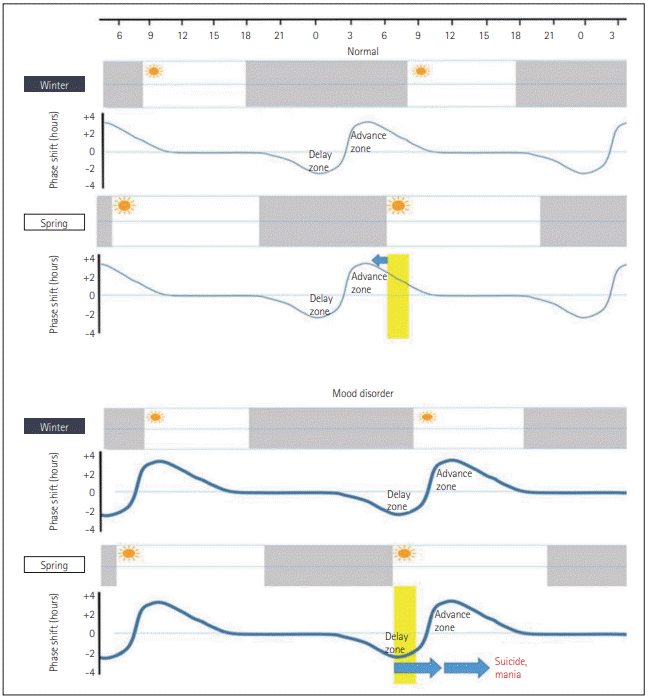
High prevalence of mania and suicide during spring explained by circadian rhythm shifting. The mechanism of increased incidence of suicide and mania in spring is explained based on the phase response curve of circadian rhythm. Modified from Cho and Lee. Psychiatry Investig 2018;15:232-234 [25].
FUTURE DIRECTION
It is still unclear whether the circadian rhythm misalignment observed in mood bipolar disorder is the cause or result of mood disorder. However, based on inference from previous findings, it is not a simple indicator of the condition that is expressed as a result of mood disturbance, but is likely to be a pathological mechanism that contributes to the development of mood disorder. Recently, my team attempted to measure and analyze objective activity parameters related to circadian rhythms in real time using a wearable device in therapeutic capacity. Using machine learning, objective indicators related to circadian rhythm were able to predict mood changes and mood episodes a few days in advance [26]. It remains to be seen whether the clinical application for prevention and treatment of bipolar disorder will be successful; however, therapeutic modalities to control the circadian rhythm should be successfully developed and applied to the treatment of bipolar disorder in the near future.
Acknowledgements
This study was supported by the Korea Health 21 R&D Project funded by the National Research Foundation of Korea (2017 M3A9F1031220 and 2019R1A2C2084158).
Notes
Conflicts of Interest
The author has no potential conflicts of interest to disclose.

